STRENGTHEN YOUR SBS KNOWLEDGE
People sometimes talk about “having a short gut,” “short gut syndrome,” or “short bowel,” but the medically accurate name for this condition is “short bowel syndrome,” or SBS for short.
Short bowel syndrome (SBS) is a serious and chronic malabsorption disorder.
SBS occurs when parts of the intestine are removed surgically and the remaining intestine may not be able to absorb enough nutrients from food and drink.
This results in malabsorption. It puts people at risk for:

Malnutrition

Electrolyte
disturbances

Dehydration

Diarrhea/
increased outputs
There are multiple factors a doctor may use to determine an SBS diagnosis, not just the length of remaining bowel.
If you have SBS, you are part of a rare and unique community. 10,000 to 20,000 people in the US are estimated to have this condition.
It is difficult to estimate the number of people with SBS in the US because it is not well documented.
Common signs and symptoms of short bowel syndrome (SBS)
When a person has SBS, their body has a hard time absorbing all the nutrients and fluids it needs to function normally. This often comes with a series of unpleasant symptoms.
New food allergies and sensitivities
Irregular stools or changes in bowel habits
Malnutrition
Difficulty maintaining weight
Vomiting
Bloating
Fatigue or sleep deprivation
Gas
Stomach pain and cramping
Heartburn
Bacterial infections
Signs of dehydration
Dark-colored urine, infrequent urination, muscle cramping, and/or excessive thirst
Diarrhea/high ostomy output
Typically more than 8 cups of fluid from an ostomy in a 24-hour period
New symptoms after intestinal surgery may point to SBS
Every person with SBS is different. You may or may not have all of the above symptoms. If you or your loved one experience any of these symptoms, talk to a doctor.
You can use this guide to start the conversation.
Doctor Discussion GuideYour doctor will evaluate your medical history and the status of your digestive system to determine the best path forward. They may ask about your symptoms, such as diarrhea, dehydration, and weight loss. They may also perform a blood test to see if you are lacking basic nutrients. Your doctor will also assess your unique nutritional needs, to give you the support you require to supplement your diet.
Need to find a healthcare provider in your area with experience managing SBS?
Find a providerTrying to describe SBS to somebody who has never been exposed to it can be difficult. I’ve always broken it down to its simplest terms: shorter intestines; having trouble absorbing food, fluid, and nutrients.”

Nutritional Support for Short Bowel Syndrome (SBS)
People with SBS may use nutritional support, depending on their remaining intestinal function
After bowel resection surgery, the lining of the remaining intestine may change to absorb more nutrients and fluid through a natural process called intestinal adaptation. Intestinal adaptation is an important goal for people with SBS. If your intestine does not adapt well enough after a section is removed, dependence on nutritional support results.
PARENTERAL SUPPORT (PS)
PS is provided intravenously (IV), delivering fluids and/or nutrition directly into a vein. Parenteral support ranges from fluid electrolytes to a complete mix of nutrients. PS can be a lifesaving intervention for some people with SBS, but over the long term it is expensive, affects quality of life, and is associated with serious complications.
Learn more about PS complicationsTotal Parenteral Nutrition (TPN)
TPN is a type of PS that provides a mixture of proteins, carbohydrates, fats, vitamins, and minerals and is customized to your specific nutrition needs. The liquid nutrients are delivered directly to your bloodstream through a large vein in your chest or arm. It is often used in the first few months following a surgery.
TPN can be a longer-term solution for some people with SBS who cannot absorb enough nutrients through their intestines. TPN can be administered at the hospital or at home (home parenteral nutrition, or HPN). Both are forms of parenteral support.
Parenteral support does not help the intestine adapt and could cause some complications over the long term.
I was on TPN for about 2 years until I could wean down, and I finally weaned down.”

Tube Feeding

STOMACH
Tube feeding, also known as enteral nutrition, or EN, delivers nutrients through a feeding tube directly into your stomach or small bowel for those with a partially functioning gastrointestinal (GI) tract. The feeding tubes are passed through the nose, mouth, or skin on your abdomen.
Tube feeding helps stimulate your digestive process and provides nutrients at a much slower rate than food taken orally. It can help maintain or improve the absorptive power of your remaining bowel, potentially offering enough nutrients and fluid to avoid the use of total parenteral nutrition. Enteral nutrition is commonly used in children with SBS.
Learn About SBS in ChildrenSBS in adults often starts with other conditions
There are many diseases and conditions that could require surgical removal of intestines, which may increase the risk for SBS, including:
This chronic disease causes inflammation and injury to the intestines. Treatment for severe cases of Crohn’s disease can include surgery.
Gastric bypass and bariatric surgery are designed to help people lose weight.
A traumatic injury to the intestine, either penetrating or blunt, such as from a car crash, may require a bowel resection.
blood vessels
Sometimes referred to as intestinal ischemia, vascular disease or injury is when the blood vessels in the intestines can’t deliver enough blood (and consequently oxygen and nutrients) to the organ to allow it to function properly.
During certain cancer treatments, it may be necessary to have tumors in the intestine removed or undergo radiation therapy.
Volvulus is a twisting of the intestine that can cause a blockage and cut off blood flow. The damaged tissue, starved of oxygen, may need to be removed via resection.
The Digestive System and Resections
Understanding what different parts of the bowel (small and large intestines) do may help explain how nutritional needs change after a bowel resection.
Whether you are about to have bowel resection surgery or you’ve already had the procedure, reviewing some basic anatomy is helpful.
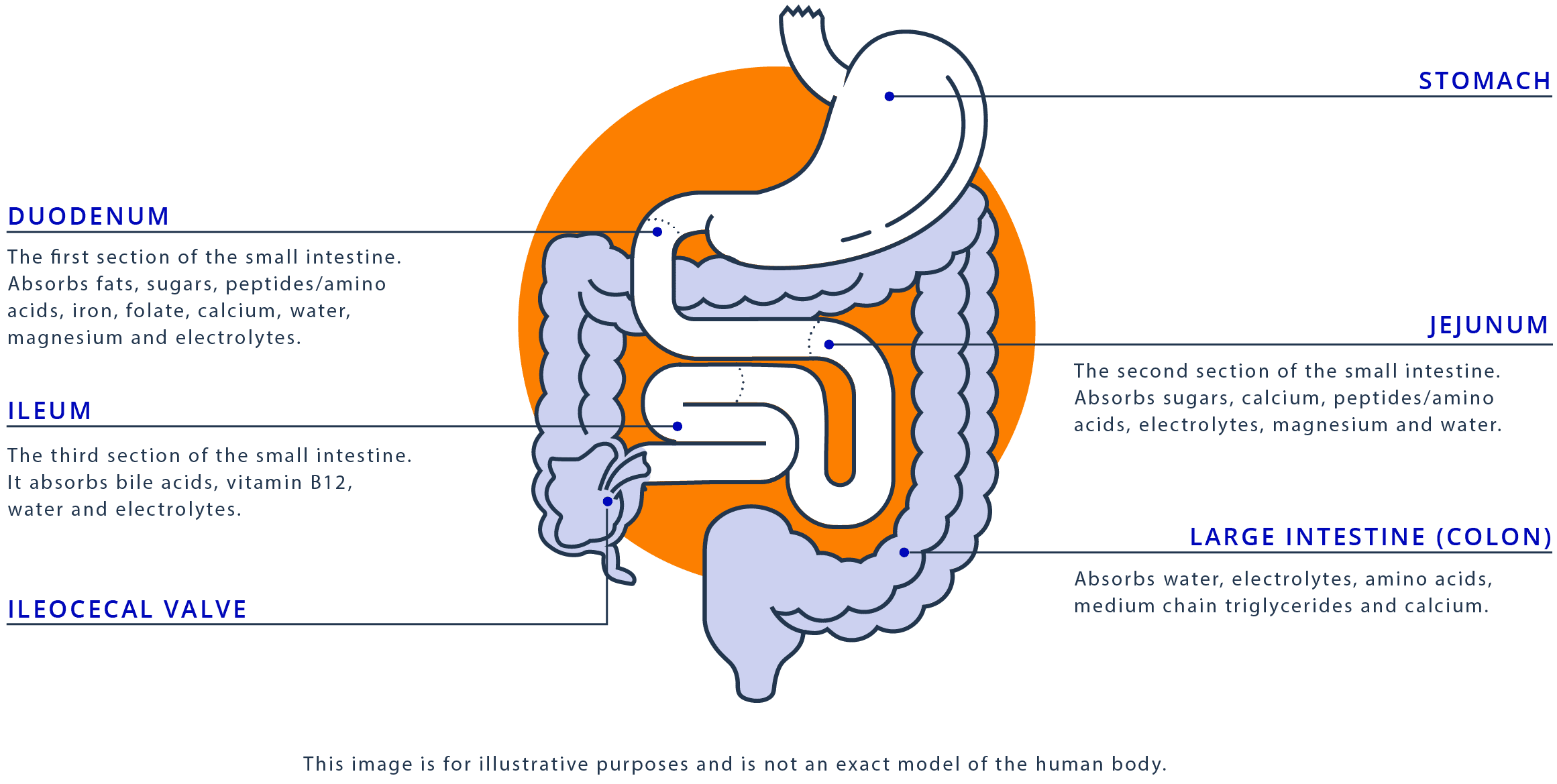
This image is for illustrative purposes and is not an exact model of the human body.
ILEOCECAL VALVE
STOMACH
LARGE INTESTINE (COLON)
Absorbs water, electrolytes, amino acids, medium chain triglycerides and calcium.
DUODENUM
The first section of the small intestine. Absorbs fats, sugars, peptides/amino acids, iron, folate, calcium, water, magnesium and electrolytes.
ILEUM
The third section of the small intestine. It absorbs bile acids, vitamin B12, water and electrolytes.
JEJUNUM
The second section of the small intestine. Absorbs sugars, calcium, peptides/amino acids, electrolytes, magnesium and water.
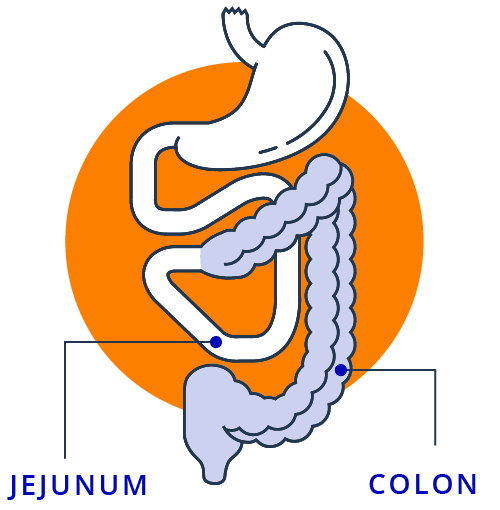
In this type of surgery, the jejunum is connected to the large intestine, also called the colon. (Anastomosis means “reconnection.”) The ileum and sometimes the muscle that joins the large intestine to the small intestine are removed. Parts of your colon may also be removed in this procedure, and the 2 sections (jejunum to colon) are then joined.
This surgery involves removal of the colon, ileum, and some of the jejunum. The remaining jejunum is then connected to a surgical opening (called an ostomy) created in the belly. The opening this creates is called a stoma. Stool or waste material goes through the stoma into a drainage bag that is located outside of the body.

In this surgery, parts of the jejunum and ileum are removed, and the remaining parts are connected to the colon. (Anastomosis means “reconnection.”) This procedure leaves the full length of the colon intact. Many people with this type of surgery do not require parenteral support (PS).
It is possible for the intestine to adapt after bowel resection surgery in some people with SBS
Bowel resection surgery may change your body’s ability to absorb nutrients from the food you eat and fluids you drink. How your nutritional needs change will depend on which part and how much of your bowel was removed and how your body adapts after surgery. This process will look a little different for everyone, but you can keep this general timeline in mind.
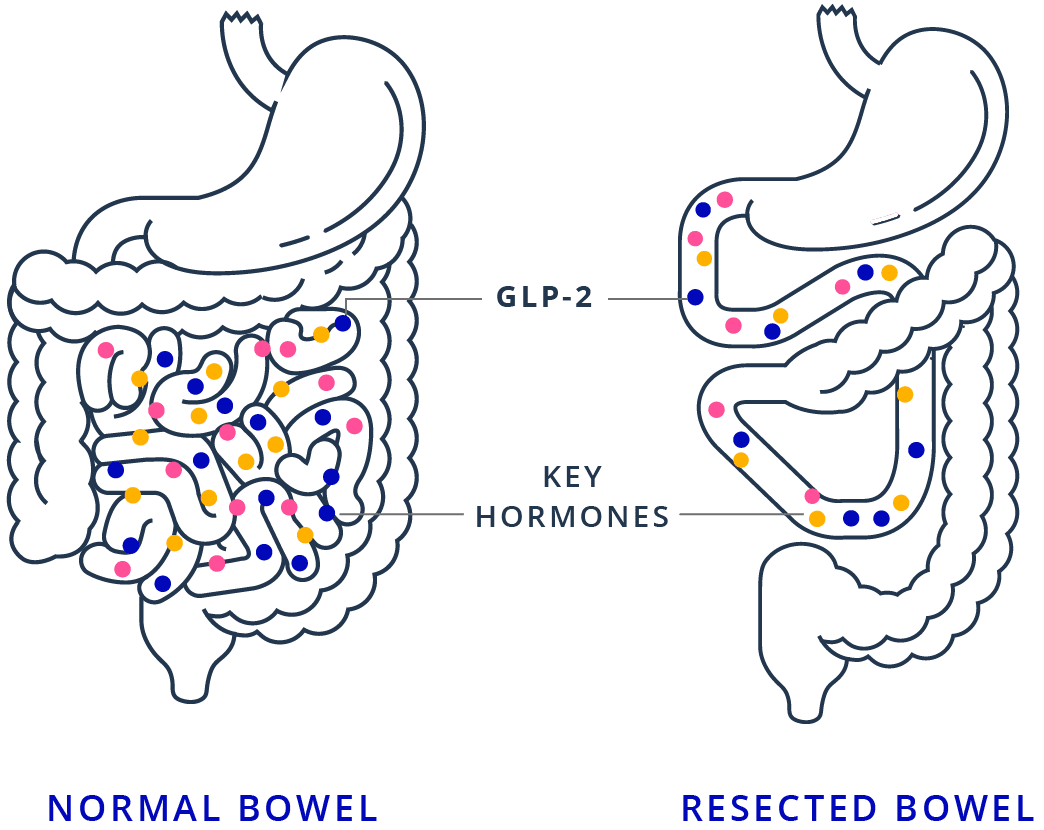
Bowel surgery can affect key hormones involved in absorption
When parts of the intestines are removed, key hormones for absorption may be affected. One example of those hormones is glucagon-like peptide-2, also known as GLP-2, which helps the body absorb nutrients or fluids. Other hormones include peptide YY (PYY) and glucagon-like peptide-1 (GLP-1). There are multiple hormones that play a role in digestion:
Peptide YY (PYY) and glucagon-like peptide-1 (GLP-1) are released near the end of the small intestine and work by slowing the transit of food through the GI tract.
In addition to slowing the transit of food, GLP-2 increases the absorptive surface area of the bowel and stimulates blood flow to the intestines. It has been shown to play a role in intestinal adaptation.
Since people with SBS have had parts of their intestines removed, they may not make enough GLP-2 or other key hormones involved in absorption.
Potential complications associated with having short bowel syndrome
Everyone’s recovery from surgery will look a little different, and you should talk to your doctor to understand your unique path forward. Notify your doctor immediately if you experience any of the following complications after surgery.
Parenteral support (PS) problems
People with SBS may receive additional nutrition intravenously. While it can be life sustaining, PS can also come with complications. These include catheter-associated bloodstream infections and long-term liver or kidney problems. Learn more about PS complications.
Vitamin deficiencies
Vitamins are essential to a healthy diet and are absorbed in the small intestines. If you have SBS, you might not absorb all the essential vitamins your body needs to function properly. Scurvy, decreased muscle coordination, and osteoporosis are all caused by vitamin deficiencies.
Mineral deficiencies
Minerals are also essential for your body to function properly, but might not be absorbed if you commonly have diarrhea. If you have SBS or chronic diarrhea, you may not absorb enough of the important minerals you need, like magnesium or zinc.
Electrolyte Abnormalities
Electrolytes are minerals that have an electric charge and play a role in the body’s chemical balance and muscular response. Some electrolytes include sodium, potassium, magnesium, and calcium. The incorrect balance of electrolytes can cause unpleasant symptoms such as headache, nausea, irregular heartbeat, and muscle weakness.
Small bowel bacteria overgrowth
After a resection, too much bacteria may grow in the small intestine. This often happens if the ileocecal valve has been removed during a resection. Bacteria overgrowth can result in gas, bloating, and diarrhea.
Kidney stones
If the bowel is not able to absorb enough calcium, fats, and bile salts, your body may produce hard crystal-like stones known as kidney stones. These do not always produce symptoms; however, “passing” the stones can be very painful.
Acidosis
Acidosis is when you have abnormally high levels of lactic acid in the blood. Undigested carbohydrates in the large intestine can lead to a buildup of lactic acid. Acidosis can cause vision problems, confusion, and/or slurred speech.
Be kind to yourself. There will be days when your mind feels good but your body’s not onboard. That’s ok. Be patient, and appreciate all the good in your life.”

Children with SBS usually have different underlying conditions, and their journey can be different.
Managing SBS can be a lifelong journey.